Why Cleaning Dental Office Environments Matters for Safety and Success
Cleaning dental office facilities goes far beyond simple tidiness—it’s the foundation of patient safety, infection control, and professional reputation. A single lapse in environmental hygiene can compromise sterilization efforts, expose patients and staff to pathogens, and undermine the trust that keeps your practice thriving.
Essential Steps for Cleaning Your Dental Office:
- Clean first, then disinfect – Remove visible debris before applying any disinfectant
- Target clinical contact surfaces – Disinfect light handles, bracket trays, switches, and drawer handles after each patient
- Use EPA-registered products – Select low-level disinfectants for routine cleaning, intermediate-level for blood-contaminated surfaces
- Maintain housekeeping surfaces daily – Clean floors, walls, and sinks with soap and water
- Follow hand hygiene protocols – Wash hands when visibly dirty, use hand disinfectant before and after patient contact
- Dispose of waste properly – Separate general waste from regulated medical waste in appropriate containers
- Keep high-touch areas pristine – Disinfect reception counters, doorknobs, and waiting room surfaces at least once daily
The stakes are clear: environmental surfaces can harbor infectious microorganisms that spread through direct contact, aerosol spray, or contaminated gloved hands. Cross-contamination from improperly cleaned surfaces exposes everyone in your practice to preventable health risks.
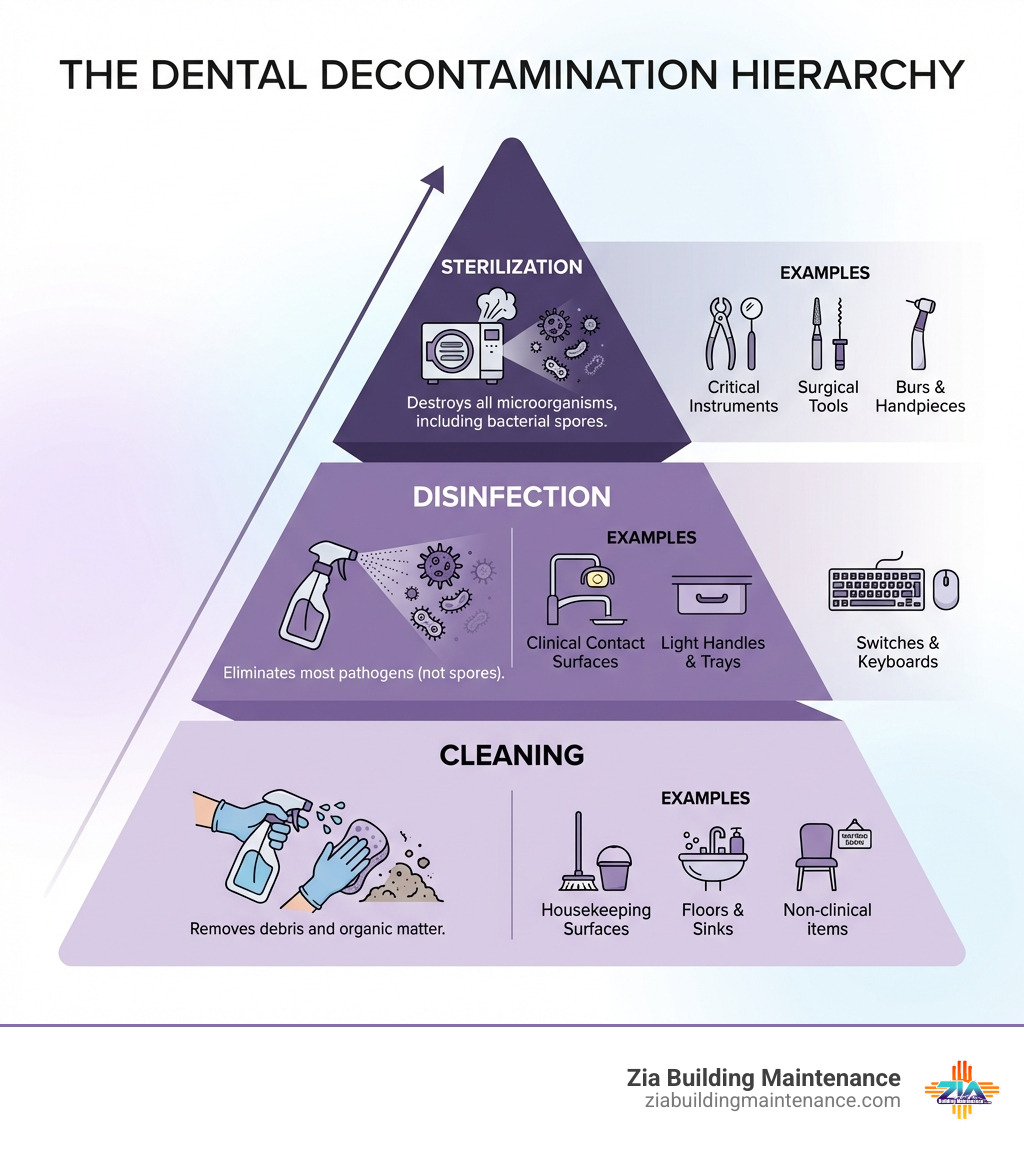
Your practice needs a systematic approach that addresses three distinct levels of decontamination. Cleaning removes organic material and debris. Disinfection eliminates most disease-causing microorganisms. Sterilization destroys all microorganisms including bacterial spores. Each level serves a specific purpose, and skipping steps compromises the entire process.
Regulatory bodies set strict standards for dental facilities. OSHA and the CDC define clear protocols for surface cleaning, hand hygiene, waste disposal, and personal protective equipment. These aren’t suggestions—they’re requirements designed to protect patients and staff from healthcare-associated infections.
I’m Ashley Cordova, and I’ve spent years helping Albuquerque businesses maintain the high standards their clients expect, with particular expertise in cleaning dental office environments where infection control is non-negotiable. At Zia Building Maintenance, we understand that your practice’s cleanliness directly impacts patient confidence and regulatory compliance.
Understanding the Core Pillars of Dental Decontamination
When we talk about maintaining a healthy dental environment, we aren’t just talking about a quick wipe-down with a paper towel. In Albuquerque and Rio Rancho, we see a variety of practices, and the most successful ones understand that decontamination is a three-headed beast.
To keep things simple, we look at the “Three Pillars” as defined by the CDC dental guidelines. If you skip the first pillar, the other two will crumble. For a deeper dive into these terms, check out our guide on The Difference Between Cleaning Sanitizing and Disinfecting.
The Decontamination Hierarchy
| Level | Action | Goal | Application |
|---|---|---|---|
| Cleaning | Using soap/detergent and water | Remove visible debris, dirt, and organic matter (bioburden) | Floors, walls, sinks, and the first step for all equipment |
| Disinfection | Using EPA-registered chemicals | Eliminate most pathogenic microorganisms (but not spores) | Clinical contact surfaces (handles, trays, switches) |
| Sterilization | Using heat (autoclave) or liquid chemicals | Destroy all microbial life, including highly resistant bacterial spores | Patient care items (instruments, burs, surgical tools) |
Why is cleaning the first step? Bioburden—that’s the fancy word for organic contamination like blood or saliva—can actually shield germs from disinfectants. If a surface isn’t cleaned first, the “bugs” can hide under the grime, and your disinfectant won’t reach them. It’s like trying to paint a dusty wall; the paint just won’t stick.
A Comprehensive Guide to Cleaning Dental Office Environments
Navigating cleaning dental office spaces requires a keen eye for detail. Not every surface is treated the same. We categorize surfaces into two main groups: Clinical Contact Surfaces and Housekeeping Surfaces.
Clinical Contact Surfaces
These are the surfaces that get “the business.” They are frequently touched by contaminated gloved hands or sprayed with aerosols and spatter during procedures. Think light handles, bracket trays, and unit switches. Because the risk of cross-contamination is high, these require intermediate-level disinfectants if blood is present, or low-level disinfectants for routine turns.
Housekeeping Surfaces
These include your floors, walls, and sinks. While they don’t usually come into direct contact with patients, they still need daily attention. Most of the time, soap and water are sufficient here. However, if a patient has a “whoopsie” and blood hits the floor, you’ll need to step up to an intermediate-level disinfectant.
For more on how we handle these specific environments, see our specialized page on Dental Office Cleaning.
Daily Protocols for Cleaning Dental Office Operatories
The operatory is the heart of your practice, and it’s also the area most prone to biological risk. High-speed rotary instruments and air-water sprays can propel microparticles containing infectious agents across the room. We call this the “splatter zone.”
Our Daily Operatory Checklist:
- Aerosol Reduction: Between patients, aerate the room to clear the air.
- Surface Barriers: We highly recommend using FDA-approved surface barriers (like plastic wraps) on hard-to-clean areas like computer keyboards and light handles. These should be changed between every single patient.
- The Wet-Dry Procedure: For non-sterilizable equipment, use an alcohol-based disinfectant. Wipe with a moist cloth, wait the required contact time, and then dry with a fresh disposable cloth.
- Waterline Maintenance: At the start of the day, flush the dental unit waterlines. Between patients, spin the turbine for at least 20 seconds to discharge any stagnant water.
For a broader look at medical environment standards, our Your Guide to Cleaning Medical Offices is a great resource.
Specialized Care for Cabinetry and Worktops
Dental cabinetry is an investment. Whether you’re in Bernalillo or the heart of Albuquerque, you want your surfaces to last. Different materials require different love.
- Durasein and Corian (Solid Surfaces): These are “renewable,” meaning minor scratches can often be buffed out. Clean them with soapy water or ammonia-based cleaners using a circular motion. Pro tip: Always run cold water when pouring boiling water into a Corian sink to prevent thermal shock!
- Laminate Care: Laminate is tough but hates acid. Avoid harsh chemicals and steel wool, which can leave permanent marks. Use a mild detergent and a soft cloth.
- Stainless Steel: To prevent rust, always rub in the direction of the grain. Chlorides left on the surface can cause pitting, so rinse thoroughly.
Regulatory Compliance: OSHA, CDC, and Waste Management
Compliance isn’t just about avoiding fines; it’s about keeping your staff and patients safe. In New Mexico, we adhere strictly to OSHA and CDC standards. If you’re worried about an upcoming inspection, our guide on How to Avoid OSHA and HIPAA Violations in Healthcare can help put your mind at ease.
Healthcare Waste Segregation
You can’t just throw everything in the same bin. Proper waste management is a statutory duty. According to the Safe Management of Healthcare Waste, waste should be segregated at the source:
- General Waste: Used masks, gowns, and gloves that are not saturated with blood can usually go in the regular trash.
- Regulated Medical Waste: Anything soaked in blood or saliva must go into leak-resistant biohazard bags.
- Sharps: Needles, scalpel blades, and broken glass belong in puncture-resistant, labeled sharps containers. Never recap a needle by hand!
- Amalgam Waste: This requires special handling. Never incinerate or heat amalgam waste, as it releases mercury vapors.
Maintaining Patient Trust in Reception and Common Areas
Your patient’s experience starts the moment they walk through your door in Albuquerque. A dusty magazine rack or a stained chair can trigger “dental anxiety” before they even see a chair. Cleanliness builds trust. You can read more about this psychological link in our article How Clean Waiting Rooms Build Patient Trust.
Reception Area Best Practices:
- Dusting: Dust all hard surfaces daily. Dust doesn’t just look bad; it can carry germs and aggravate respiratory issues.
- Clutter Removal: Keep the desk clear. Neatly display magazines or, better yet, switch to digital entertainment to reduce high-touch surfaces.
- Furniture Maintenance: Check for tears or stains daily. If it’s fabric, it needs regular professional cleaning; if it’s vinyl, it needs a daily wipe-down.
Maintaining Hygiene when Cleaning Dental Office Restrooms
Let’s be honest: patients judge your clinical skills by the state of your restroom. If the bathroom is messy, they’ll wonder if your instruments are, too.
Our Bathroom Cleaning Service focuses on:
- Stocking: Ensure toilet paper, soap, and paper towels are always available.
- Disinfection: Use EPA-registered disinfectants on faucets, flush handles, and door locks.
- Odor Control: A clean bathroom shouldn’t smell like perfume; it should smell like nothing. Odors are usually caused by bacteria, so kill the bacteria, and you kill the smell.
Hand Hygiene and PPE: Protecting Staff and Patients
Hand hygiene is the single most important practice to reduce the spread of germs. The 2024 updates to the Code of Practice on the prevention and control of infections emphasize that hand hygiene must be performed at key stages: before patient contact, after contact with the patient’s environment, and immediately after removing gloves.
The Zia Hand Hygiene Protocol:
- Wash with soap and water for at least 20 seconds when hands are visibly dirty or after using the restroom.
- Use alcohol-based hand sanitizer (at least 60% alcohol) for routine decontamination if hands aren’t visibly soiled.
- No jewelry: Keep those wrists and fingers clear of rings and watches, which can harbor bacteria.
Personal Protective Equipment (PPE)
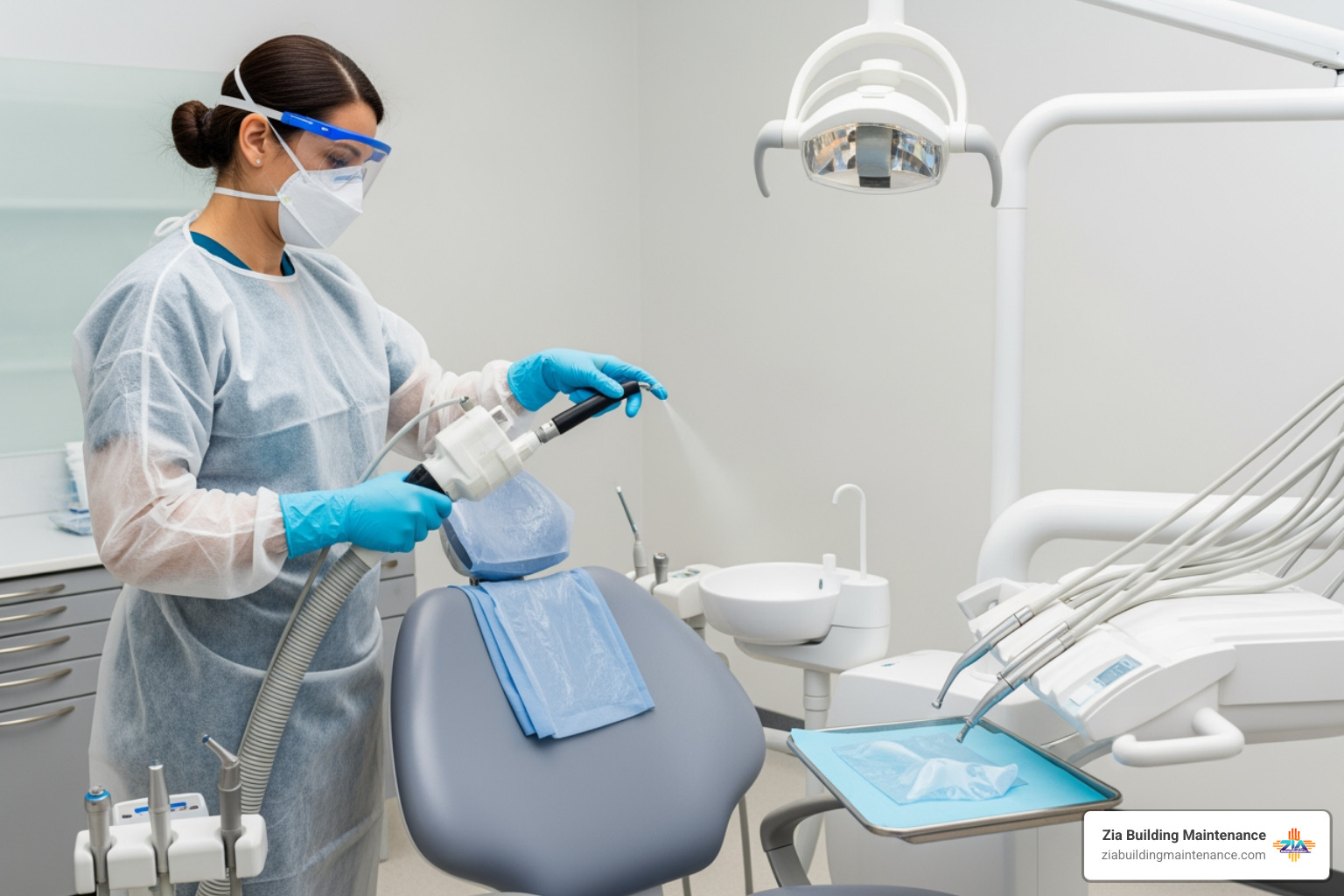
When cleaning dental office operatories, staff should wear more than just patient-exam gloves. We recommend chemical- and puncture-resistant utility gloves for handling disinfectants and cleaning used instruments. Protective eyewear and surgical masks are essential to prevent splashes from reaching your mucous membranes.
Frequently Asked Questions about Dental Office Cleaning
What is the difference between low-level and intermediate-level disinfectants?
Low-level disinfectants are EPA-registered and effective against most vegetative bacteria and some viruses (like HIV and HBV), but they don’t kill mycobacteria. Intermediate-level disinfectants have a “tuberculocidal” claim. This doesn’t mean we’re worried about catching TB from a chair; it’s just a benchmark. If a chemical can kill the tough Mycobacterium tuberculosis, it can kill almost any other common pathogen.
How often should dental unit waterlines be flushed and treated?
You should flush waterlines every morning for at least two minutes and between patients for 20-30 seconds. Additionally, the water quality should be tested regularly. The goal is to keep the bacterial count below 500 CFU/mL (the standard for safe drinking water).
What specific PPE is required for cleaning the dental operatory?
For cleaning and disinfection, you should wear heavy-duty utility gloves, a fluid-resistant gown, a surgical mask, and protective eyewear (goggles or a face shield). Standard exam gloves are often too thin and can be degraded by the chemicals in disinfectants.
Conclusion
Maintaining a pristine dental practice in Albuquerque, Rio Rancho, or Bernalillo is a full-time job that requires expertise, the right tools, and a commitment to safety. At Zia Building Maintenance, we’ve spent over 30 years perfecting the art of the “truly clean” space. We know that in a dental office, a missed corner isn’t just an eyesore—it’s a risk.
By following a systematic approach to cleaning dental office surfaces, staying compliant with OSHA and CDC standards, and prioritizing patient-facing areas like the waiting room, you can ensure your practice remains a safe, welcoming, and professional environment.
If you’d rather focus on your patients’ smiles and leave the heavy lifting to us, we’re here to help. Our family-owned team provides the dependable service and attention to detail that Albuquerque healthcare providers have trusted since 1989. Let’s keep your practice pristine together. Check out our Dental Office Cleaning services today!